Updated June 6, 2021
I’ve seen two new patients this week that made me mad. Not because of anything the owners or patients said, but the advice they received.

“He’s too old to have an anaesthetic. It’s too dangerous.”
What utter poppycock. These poor animals were living with painful and easily treated problems.
However, before I carry on ranting, please stop me to remind you that these attitudes are increasingly rare . Nearly all vets will agree with what I am about to say.
That is: Age is not a disease. What matters is your pet’s health status.
There are a few common myths we hear about anaesthetics:
- Too many anaesthetics are dangerous. Each anaesthetic is independent, and there is no cumulative effect if the effect of the last drugs have worn off. This can be within a few days.
- You can’t anaesthetise sick animals. If this was true it would be very bad news for many dogs we see.
- Anaesthetics aren’t safe in old animals. Ditto.
- Sedation is safer that anaesthesia. Not always. The airway is controlled by an ET tube under GA, and gaseous anaesthetics are easier to control and monitor.
So What Does Make Anaesthetics Risky?
No question, sometimes we will advise you avoid an anaesthetic. Here’s when:
- No recent checkup. We could be sleepwalking into a disaster. Please understand if we ask for another checkup before surgery if it’s been too long.
- Untreated diseases. These can include anaemia, heart disease, cushing’s syndrome etc. I have no trouble with anaesthetising these animals once they are treated.
- Very young or underweight animals who can rapidly lose body heat or suffer low blood glucose.
- Repeated unnecessary or cosmetic procedures. Don’t worry: we’ll give our honest opinion. However, if a dog needs daily anaesthetics (for example for burns dressing changes) we can do it. We just don’t want to do it needlessly.
- Or simply if we haven’t enough nurses to monitor. That’s why we won’t do routine procedures on Saturdays or after 5pm. Sometimes we’ll even reschedule procedures if nurses call in sick.
What Can Vets Do To Make Anaesthetics Safer?
- Thorough patient evaluation. We don’t perform a pet anaesthetic without a recent, full physical examination. We need to know about cardiovascular and respiratory function, plus any other health issues that may be relevant. Often we will defer an anaesthetic until we have investigated or stabilised a problem we find.
- Preanaesthetic blood testing. This simple and inexpensive test will identify a wide range of hidden diseases. We recommend testing on all animals, but if we see a specific reason for concern, our recommendation will get a little pushier.
- Planning. Each patient is different, and anaesthetics are tailored to suit each animal’s needs.
- Trained and motivated staff. Our greatest resource is our nurses. They have to be highly trained and updated, and empowered to have their concerns listened to.
- Heat conservation. Our nurses not only wrap their patients before surgery, they also bed them on a forced air patient warmer. This is really effective. By doing this we can prevent significant heat loss in almost all animals.
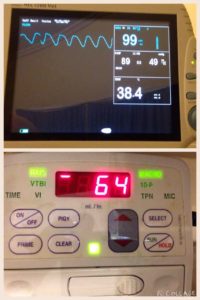
- Up to date monitoring equipment. We routinely monitor blood oxygen saturation (pulse oximetry), blood pressure, heart rate, respiratory rate and core body temperature.
- Fluid therapy. All our patients receive intravenous fluids during their anaesthetic, to maintain blood pressure and provide a quick route for emergency drugs.
- Post operative monitoring. In a recent UK survey*, although total deaths were small, over half of these occurred after the operation had finished. We have strict monitoring protocols to ensure a patient is never left alone after surgery.
It may help you to know that most of our anaesthetics (except desexings) are in elderly patients. Old animals do get more health problems. Rather than that being a reason to not give them anaesthetics, it actually means we need to do it more often to maintain their wellbeing.
Anaesthetics are a wonderful invention. Ever since Queen Victoria used them for childbirth, anaesthetics have saved animals and people from immense pain and suffering. Nowadays, pets get similar drugs and monitoring to human anaesthesia. Risks exist, but they can be minimised by following simple protocols. The next time your pet needs an anaesthetic, trust the vet if they tell you the risks are small. They care deeply about their patients and only want what you want: a pet with the best quality of life they can get.
*Brodbelt, D. C., Blissitt, K. J., Hammond, R. A., Neath, P. J., Young, L. E., Pfeiffer, D. U., & Wood, J. L. (2008). The risk of death: the confidential enquiry into perioperative small animal fatalities. Veterinary anaesthesia and analgesia,35(5), 365-373.
Have something to add? Comments (if open) will appear within 24 hours.
By Andrew Spanner BVSc(Hons) MVetStud, a vet in Adelaide, Australia. Meet his team here.

