Updated September 13, 2022
Lymphoma in dogs is unfortunately quite a common cancer. It happens when the white blood cells called lymphocytes start growing and multiplying uncontrollably. They then spread to the lymph nodes, blood or internal organs.
A rare form that targets the skin is epitheliotropic lymphoma (EL), also called mycosis fungoides or cutaneous lymphoma. It has a very different appearance and outlook.
Signs Of Epitheliotropic Lymphoma
Epitheliotropic lymphoma is very difficult to diagnose and is often overlooked for some time. The lesions are not specific and look like any other severe skin disease. Signs may include:
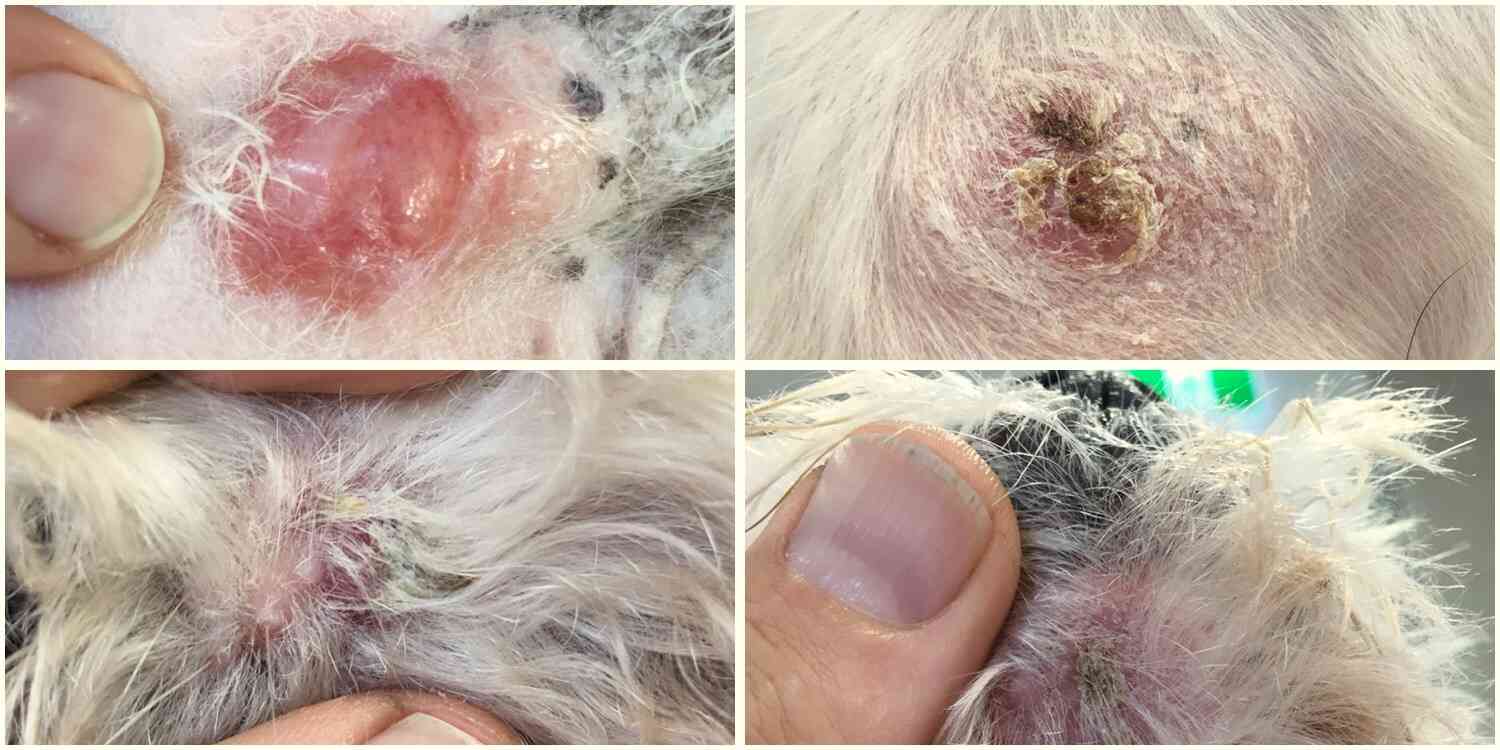
- Widespread red and scaly skin
- Areas of raised red nodules and scaling
- Ulcerated and depigmented patches
- Severe itch
There is usually a very poor response to the first attempts to treat based on more common conditions. At this point, the diagnosis is usually made via a surgical biopsy.
Treatment of Epitheliotropic Lymphoma
Treatment options include:
- Surgical removal of solitary lesions (not recommended for multiple sites)
- Radiotherapy (not available in Adelaide, not always useful)
- Chemotherapy (see below)
- Retinoids (isotretinoin, acitretin) daily
- Safflower oil (3mL/kg daily)
- Soothing creams (we find Aloveen conditioner works the best)
Chemotherapy for EL has traditionally been the use of lomustine (also called CCNU) every 3 weeks. Recent evidence suggests that combination chemotherapy (called ‘VELCAP-EL’) may produce longer survival times, however side effects are also likely to be more common.
Prognosis Of Epitheliotropic Lymphoma
Current treatment does not provide a very good prognosis. Chemotherapy provides a much lower benefit than we see with other forms of lymphoma, but it does help to reduce signs of illness. Survival times with treatment are only around 6 months.
Chan, C. M., Frimberger, A. E., & Moore, A. S. (2018). Clinical outcome and prognosis of dogs with histopathological features consistent with epitheliotropic lymphoma: a retrospective study of 148 cases (2003–2015). Veterinary dermatology, 29(2), 154-e59.
Have something to add? Comments (if open) will appear within 24 hours.
By Andrew Spanner BVSc(Hons) MVetStud, a vet in Adelaide, Australia. Meet his team here. The information provided here is not intended to be used as a substitute for going to the vet. If your pet is unwell, please seek veterinary attention.

Our Labbie was diagnosed with EL about six months ago, but she’s had multiple tumors surgically removed for a year now. She has been on high doses of Prednisone and the effects are awful, although it did initially help with decreasing the size of the lesions. She now has no strength in her back legs, her lesions have ulcerated, and her muscles are wasting away. Her head is just skin and bone. Our vet says she’s lasted longer than any of the other dogs he’s seen with this disease – he’s only seen five cases in his 30 years of practice. We’ve decided to put her sleep next week as she’s just declining. I’m heartbroken.
My 9 years old pup has been diagnosed with it (biopsy) – and I am heartbroken but somehow still hope they were wrong…. He developed “skin tags” last year, one of them was oozing non stop and bleeding and didn’t heal. He had surgery to remove it approx 11 months ago. He developed scabs all over his abdomen shortly after. Obviously, it was identified as allergies, then as bacteria, then he had antibiotics and prednisone, then we stopped the prednisone and they got much worse, affecting other areas. Altogether, it took approx half an year from the development of scabs to the biopsy and diagnosis. Now that we went through the biopsy and we know what he has, he has been given Prednisone again and the scabs healed, he eats like a horse, jumps around, plays with his toys, chases cats and seems absolutely fine…?! He drinks and pees a lot, but then this was the case before when he was on Prednisone. Other than that, he seems absolutely fine. Is this normal, 11 months after the first lesion? Is there any chance that he actually doesn’t have it – or by some miracle he has a variant with a very slow development?! I may hope against hope here, but he’s really doing very well – and doesn’t have any discomfort anymore.
Hi Don. Your story sounds fairly standard, and I would therefore expect that the diagnosis is correct. There’s always a chance that pathologists are wrong, but it would happen less than one percent of the time.
I have a 4 month old golden just diagnosed with EL. He had an eyelid tumor removed by an ophthalmologist and biopsy done. With a growing puppy do you suspect this disease will move faster in his body? I have had him 4 weeks today and wondering if I should give him back to breeder or need to understand what to expect.
Hi Merrill. Unless the disease is different in puppies, it is a relentless horror, and if you can talk to the breeder that would be very wise. This tragic event fits with my complaints about the rate of cancer in the breed that you can see here.
Why would you give him back to the breeder? Love him as your own. Make the breeder aware of the diagnosis.
My 10 yr old goldie was diagnosed with this early this year and was treated with roacutain because we caught it so early, it’s worked great and she’s been fine now they are progressing and we’re really not sure that chemo is the way to go as what she would have to go through we feel wouldn’t be fair on her
I’m so sorry to hear! My dogginjust got diagnosed with EL. Which kind of vet prescribed roacutain?
My 14 year old Shih Tzu has EL. The only presentation of it was a red lesion that appeared as a scab on her tiny paw pad by her elbow, that suddenly grew to the size of a marble, turned red, and started oozing. It was surgically removed and biopsied. She just received her third round of CCNU. How to do determine if CCNU is effective when the only presentation of EL was already removed? She never had swollen lymph nodes so we can’t determine by that. She continues to develop little red bumps with a layer of dandruff over her body, however they believe this is normal old dog warts, however what I read online suggests it might be EL.
My 14 year old Golden Retriever was diagnosed by biopsy in July. She has about 12 lesions now but after starting steroids they are all flat again. The initial three were half dollar size and raised up. She then quickly got three tumors on her lips which grew dramatically within days, (before steroids). They are all shriveled now too. However, she is still getting more lesions on legs and new one on bottom of paw. She is chewing her wrists and forearms, one until it bled, and one back foot. Her skin on those three legs is turning black. I think she may have developed Cushing’s from the steroids? She also has intermittent blood in some stools. Her hind legs have gotten very weak and she slips and slides on floors without carpet. She drinks all the time and I have to let her out 10-12 times a day. She pants heavily all the time. Vet gave Gabapentin to see if it would help with itch and pain, (200 mg day), but not helping. Is it time to let her go? Is she suffering too much? Steroids is 20 mg day. Oh, and very good aggressive now..bit me bad Friday when trying to give her meatball with pill. My thumb was impaled by her canine tooth and couldn’t get it out for about a full minute. Had to get tetanus shot and antibiotics for myself..still hurts as it hit the nerve!
Mary
Hi Mary. I’ll give a few general comments and then a conclusion. Firstly, that dose of steroids is quite low and unlikely to cause Cushing’s. It’s even possible that more would improve her symptoms but I would call that a long shot. Secondly, the dose of gabapentin is also quite low and could easily increase with your vets guidance. Again, it may make very little difference.
In essence, EL is a vale of tears and has very few good stories attached to it. In your case, yes, I think it’s time to let her go. Not just from your description, but from the aggression which I am sure is highly out of character and probably related to her discomfort.
Hi there, my 11 year old labradoodle was diagnosed back in 2017 ( when she was 7) . I put her on a raw meat diet and add olive leaf extract to her meal every day. It’s four years later and even though the lesions are popping up at a faster rate now we are still managing them with comfrey ointment and occasionally paracetamol ( when they irritate her -it helps to stop her nibbling them ).
I have seen them go from red/black,angry,painful ,weeping lumps to totally healed over with hair regrowth. Don’t give up!
Hi Dawn. That’s amazing. In fact, so amazing that I need to ask – did she have surgical biopsies done to confirm the diagnosis?
I definitely needed to read your reply!
Hi Dawn, it has been a while but asking is worth a shot to ask here. My senior lady is going through this journey like a champ. Yesterday I cleaned up one of her scabs which was leaking when pressed and it was red underneath, today the little layer of discharge from the skin has started to crystalize a little and it is a little shiny/wet in the center of the lesion. I am not sure how to go about cleaning or treating these red lesions, if anything should/could be applied to soothe. Is this where you apply the comfrey ointment? I am just looking to see what I can apply to soothe the red lesions a bit if possible, she is not itchy and I am thankful for that grace.
My 10 year old golden retriever was diagnosed with Epitheliotropic cutaneous lymphoma in January after finding little tiny nodules on his back and his tail. He quickly started to lose pigment in his nose and he was extremely tired. We started the lomustin every 3 weeks – did 3 treatments over 3 months. First 2 worked; last one didn’t have any effect and he went downhill fast. When he was on the prednisone he had to be taken off the meloxicam for his arthritis and his arthritis got so bad. We had to put him down after he stopped eating, couldn’t get up, back legs no strength at all. It was terrible. It is a bad disease – and the one thing that bothers me is that before the 3rd treatment, his blood tests said he was doing fine – I’m not sure how that could be. I am heartbroken, loved him so much. This is a very serious cancer; are there any causes? It affects so few dogs.
Hi Dee. Yes it’s a heartless disease. The cause isn’t known, and most dogs follow a similar course to yours. Blood tests often don’t show much even when it’s making the dogs feel quite unwell.
Hi Andrew. Our 12 year old Whippet x fox terrier has just been diagnosed with EL after 5+ months of lesions which had been diagnosed by 3 vets as a food allergy. We have been treating her with low dose prednisolone (5-10mg daily for about 4 months) and the Canine anallergenic prescription food. She has hideous lesions on the anus, genital area, one nipple, face and a couple of other red patches over her skin, as well as marked and sudden onset of white spots on her limbs, on what has always been jet black fur.
Her bloods were normal, she is otherwise well in herself – eating drinking, running around when not sleeping. She does lick the anal lesion quite a bit so we tell her not to (and she stops immediately) and we sometimes put nickers on her to prevent access.
We think we would prefer not to engage her in chemo as we are worried about making her sick, and needing monthly visits to the vet 30 mins drive away to be poked and prodded. We have now been prescribed Prednisolone 15mg once daily for 2 weeks and then 15mg 2nd daily.
What are your thoughts on us not opting for Chemo? I have not come across any scientific papers that evidence benefit from Chemo for this condition.
Also what symptoms would likely indicate the end of life is near for her?
Thank you for this blog. Kirstie
Hi Kirsty. My experience with using chemotherapy for EL is limited to 2 dogs but having also looked at the literature and spoken to our local oncologist I think it is a reasonable decision to not pursue chemotherapy. EL is a horrible disease with poor response rates and so not using these drugs is not a case of depriving a dog of a cure. Yes, there is likely to be improvement in the survival time but this is measured in months. We have to weigh up the reasonably high chance of side-effects that will occur during treatment.
Having said this, for most susceptible cancers I usually do go for chemotherapy but then stop it quickly if the dog is not coping well. In your case with the distance to travel that might swing the decision. As for the end of life, like with so many chronic diseases, it’s often best judged on your dogs attitude and joie de vivre. As long as they maintain their happy self and perform all their normal daily routines with the same gusto, no matter how bad the lesions look they are probably feeling fine. However, once they start withdrawing or becoming subdued I would worry a lot about proceeding.
I know this is an older post but I just wanted to share my experience with chemo for my pup.
I had a super sweet Schnauzer who developed Cutaneous Lymphoma (which was initially diagnosed as allergies by a vet, so I ended up taking her to a dermatologist who diagnosed her accurately). We opted to try Chemotherapy…so a few days after the first treatment she started having side effects from the chemo. Mostly vomiting and nausea. Well she ended up with aspiration pneumonia from the vomiting and quickly got worse, then had a seizure right after another vomiting episode and became comatose, so we had to end her suffering and had a mobile vet come to the house to let her go. It was so incredibly traumatic and beyond heartbreaking to go through that and see her suffer through the side effects of the chemo. I would never do chemo again on any of my pups because of that awful experience 🙁 I felt that the prednisone seemed to help make her more comfortable and we should have left it at that…
Hi Andrew, my recently diagnosed 11yo Mini Foxy boy has Cutaneous Epitheliotropic Lymphoma and so far only one skin lesion and a nearby lymph gland and an ultrasound indicates it hasn’t spread to other sites, though could be microscopic. I always said I wouldn’t put a dog through chemo because they won’t know why they are feeling so badly from the side effects. But my vet (and Dr Google) told me the chemo doses for dogs are much lower than humans as the aim is not to cure it but to reduce symptoms and extend life by months, or even a year. Which for a dog who is 11 even an extra 6 months of good quality life is a lot. For him and me.
I think this is worth pointing out to people whose dog has just been diagnosed with a cancer and they are weighing up the options, trying to do what is best for their dog, who has no understanding of the condition or treatment. I’ve opted to go with surgery + chemo.
My sweet little dog was just diagnosed. As you indicated, he has been treated for numerous skin lesions, for many months, with no improvement. The results of his biopsy just came in and I am devastated. He is a nearly 10 year old pug and I can’t bear to watch him suffer. He has been given a steroid shot for itching, is taking antibiotics, and is on pain medication. I have opted not to do chemotherapy. I would welcome suggestions on, at what point, is euthanasia recommended? I don’t want him to suffer.
Hi Kim. It’s reasonable to try chemotherapy, as a proportion do very well. However, euthanasia is best when there’s clearly no improvement or at the first signs of relapse. Without chemo, I would not persist for long at all as these poor dogs will inevitably worsen.
My dog has some sort of a bit bloody smooth pink ball on neck. There is 2. It looks very bad..i can’t believe i didn’t notice it. It is outside of his body. Is it something really bad?
Hi Tamara. Only a checkup at the vet can answer your question I’m sorry.
Thank you for your info. Our 8.5 years old Border Collie has today been diagnosed with the C E L having had a huge lump removed from under the skin near his nose. He had no signs of this illness apart from the lump which appeared 3 months ago, until his lymph node was swollen. The first biopsy was unclear. Our Vet said we could think about chemo but he didn’t sound hopeful about it. He suggested we do our own research then get back to him.
My Dog has some of these sores on her will she die from this and if so what can I do. Dogs name is Angel . Thank you
Hi Marie. EL is so rare that it’s almost certainly something else a lot better. Get your vet to take a look.